We here at the CODRA Hospital spinal surgery center have the state of the art equipment at our disposal and use the contemporary work procedures in order to deal with discus hernia and other degenerative spinal diseases.
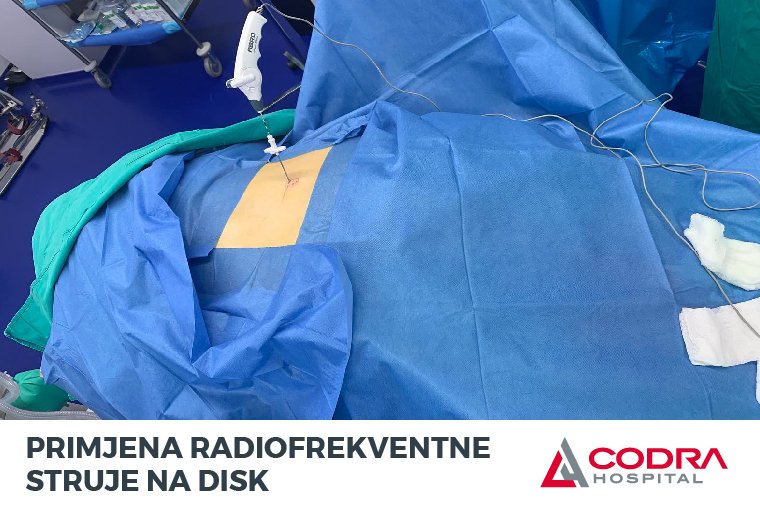
It is also possible to solve the problem of disc herniation without a surgical incision, using radiofrequency current under local anesthesia.
Disc herniation is the result of degenerative changes that lead to wear or damage to one or more discs. Displacement of the intervertebral disc into the spinal canal often leads to pinching and inflammation of the nerve with severe pain in the neck or back that often spreads down the arm or leg. The patient may also feel muscle weakness, tingling in the arms or legs and the lower part of the spine.
Minimally invasive techniques for the treatment of disc herniation and other degenerative diseases of the spine include techniques that, with minimal tissue trauma, achieve the maximum effect. The advantages are faster return to normal life activities, no scar, pain removal.
The diagnosis is established based on an X-ray image, a scanner image and a clinical examination. When conservative therapy does not provide satisfactory results, a neurosurgeon is consulted in order to determine whether there is an indication for one of the surgical treatment methods (such as endoscopic or microscopic spine surgery) or for one of the minimally invasive methods (PRDD).
PRDD – percutaneous radiofrequency disc decompression is a modern procedure that has many advantages:
- It is done under local anesthesia
- Fifteen minutes procedure
- Tissue trauma and bleeding are minimal
- No scar
- Quick removal of the pain
- Short recovery process
- The patient can go home one hour after the intervention
Prior to the surgery it is necessary to determine the exact location of the prolapse i.e. the location where the cartilage tissue exited the spinal canal and pinched the root of a nerve in the spinal column.
Most frequently, patients suffer from pain in the lower back, which is caused by prolapse at the level of lumbar vertebrae L4-L5 and/or L5-S1. An X-ray, scanner or MRI provides accurate localization.
The procedure begins with administering local anesthesia. Then a probe that conducts radiofrequency current is passed through the hole in the skin. The energy released by the radio frequency current is applied to the disc, so that it shrinks and the pinched nerve is relieved of pressure (decompression process).
Endoscopic surgeries are also superior because they provide maximal visualization and minimal tissue trauma, minimal bleeding and minimal scarring.
With the constant improvement and advancement of arthroscopic methods in all branches of medicine, with the help of endoscopes, these procedures are becoming more and more popular. Endoscopic discectomy is the only true minimally invasive surgery that achieves the maximum effect of nerve decompression with minimal tissue trauma. The obvious advantage of this procedure is direct visual control of local structures and less tissue traumatization. Compared to other procedures, these procedures are technically demanding and are performed with a number of appropriate accessories. Precisely these types of access were often difficult and limited by degenerative changes (e.g. spondylophytes), which is no longer the case today with the development of modern instrumentation. The CODRA hospital has the most modern equipment for performing these procedures.
Complete endoscopic discectomy is performed under local or general anesthesia, where the endoscope is introduced through a seven to eight millimeter incision to reach the place of nerve compression, which is pressed by a herniated disc or some other degenerative process.
The most important difference to the conventional operative procedure is the lateral access through the foramen, ie. transforaminal approach. In this way, the spinal canal itself is avoided, the nerves remain completely intact, therefore excluding the possibility of injury, epidural scar, adhesion and other complications that follow classic surgeries. There is no possibility of instability because the intervertebral ligaments that stabilize the spine remain intact.
Transforaminal approach is done under local anesthesia through a small 7-8 mm incision, through which an optical endoscope is introduced with a view to reach the intervertebral disc. Almost immediately the prolapsed disc material can be removed under visual control. After that, the space through which the disc came out is “welded” (with bipolar radiofrequency energy) and the pain receptors are modulated at the same time. For the revitalization of the spinal disc, autologous bioregenerative serum can be administered. The duration of the intervention itself is usually 30 to 45 minutes. The patient is discharged either on the same day or after a monitoring period of 24-48 hours.
The endoscopic technique does not require a large incision or a wide opening of the spinal canal. With the incision being just a few millimeters wide, the risk of postoperative scaring is minimal. There is almost no tissue destruction. The duration of the surgery is significantly shorter compared to the old school procedure, the healing process is accelerated and the recovery process is significantly shorter. Due to the shorter duration of the procedure the postoperative risk of infection is reduced to a minimum. The patients that underwent this type of surgery experience a significantly lower level of postoperative pain, are mobile right after the surgery, and the recovery period is significantly shorter when compared to the open surgeries.
Candidates for this type of minimally invasive surgery are patients with clear indications, as well as for open surgery, with certain differences – radicular pain that does not go away after applying conservative treatment for more than 6-8 weeks, or the presence of a neurological deficit,caused by nerve compression due to intervertebral disc prolapse.
Bioregenerative medicine is particularly popular in recent years. It is known that the natural process of disc aging includes desiccation, i.e. loss of water, collagen and proteoglycans. The disc becomes brittle, altered and susceptible to exit into the spinal canal where it exerts pressure on nerve structures. Bioregenerative autologous serums, such as Orthokin, work in two ways: they reduce inflammation by blocking inflammatory mediators due to the presence of cytokines and help regeneration by stimulating the synthesis of collagen and growth factors (TGF-β). Ortokin serum is obtained by processing blood taken from the patient himself. With the same goal, his own stem cells or various hyaluronic and chondro-collagen can be administered. The application process itself is done in an OR using the transforaminal technique with fluoroscopy control, and lasts a few minutes.
The patient is discharged about an hour after the intervention and he can go back to his day to day activities. The treatment is continued through physical therapy.
Vertebroplasty is an intervention that effectively and quickly resolves a vertebral fracture in awake patients, without a classic incision, in the case of vertebral fractures that occur, most often, due to osteoporosis in women. The procedure is performed under local anesthesia and lasts about 30 minutes. Instead of a classic surgical incision, percutaneous vertebroplasty is performed by inserting a special needle through the skin. The broken vertebra (or more) is found with X-ray and bone cement is inserted into it, which works by stabilizing the altered vertebral body, which leads to a reduction in pain. As soon as the vertebra is filled, the pain is reduced or completely removed. Recovery is fast, and by applying this method, people who could not tolerate general anesthesia can now be treated.
At the CODRA Hospital all types of procedures and minimally invasive treatment techniques for disc herniation and other degenerative diseases of the spine are performed by Dr. Sci. Med. Nenad Živković, specialist in neurosurgery, spinal surgeon and scientific associate, with the view to implement new global trends in the treatment of spinal pathology in Montenegro, which he largely mastered and perfected by working with some of the world’s best experts in this field. Dr. sci. Med. Nenad Živković has over 50 published scientific papers in the field of neurosurgery, as well as two books, one of which was published in Germany.